Genital herpes is one of the most commonly sexually transmitted diseases which is caused by the Herpes Simplex Virus (HSV).
This can be associated with chronic recurrent urinary tract symptoms such as dysuria (painful urination), urgency, and frequency. This could be a type-specific for type 1 and 2 genital herpes that one might have as most cases of genital herpes are caused by infection by the herpes simplex virus type 2 (HSV-2).
Herpes simplex virus type 1 (HSV-1) is more often the cause of cold sores or fever blisters but it can also be a cause of genital herpes.
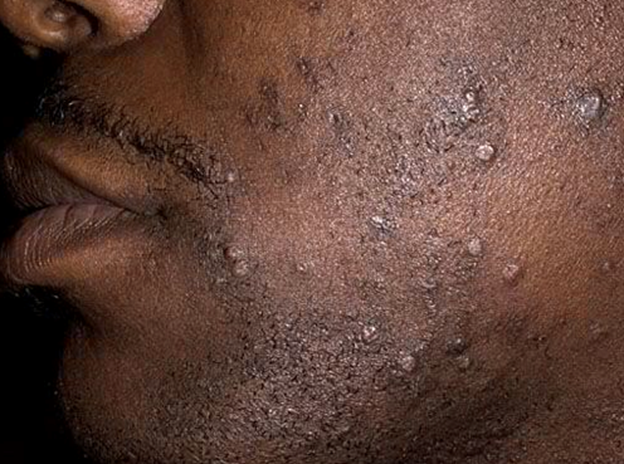
Unfortunately, if patients have symptoms of herpes, they are often an atypical where one complains or shows symptoms of urinary tract or chronic yeast infection.
Clinicians consider genital herpes in the differential diagnosis of chronic dysuria which refers to painful urination, particularly when the urine cultures are negative.
Most people with genital herpes don’t know they have it as in most people it produces either no symptoms or very mild ones.
What Happens in an HSV Infection?
Genital herpes virus is passed from one person to another through sexual contact. This happens even if the person with the virus doesn’t have symptoms or signs of the infection.
Once the virus enters through the skin , it travels along nerve paths and it may become dormant (inactive) in the nerves and remain there indefinitely.
One could have briefly learned about sexually transmitted infection(STI) and urinary tract infection (UTI) in high school health, but probably weren’t clued in to how common both these kinds of infections are and how similarly they can feel.
Both these kinds of infections are relatively common considering how close the reproductive organs are to the bladder and urinary tract, telling the difference between a UTI and STI can be difficult at times.
However, there are slight differences in these two types of infections that an obstetrician and gynecologist can say you can spot on your own regarding that an STI can feel quite similar to a UTI because the infection too can often be felt as burning, pain upon urination, and pelvic pain.
Though it’s totally possible to have an STI and present no obvious symptoms burning and painful sensations that feel similar to a UTI, the two are not out of the norm from differentiating between herpes, chlamydia, or gonorrhea, versus a UTI is typically the most challenging at home.
From time to time, the virus may become active and when this happens, the virus travels back along the nerve path to the surface of the skin, where additional virus is shed. At this point the virus may cause an outbreak of symptoms or it may remain undetected.
Symptoms?
In either case, the active virus is easily passed from one partner to another through sexual contact even wearing a condom may not protect the uninfected partner. The virus can be present on skin that remains uncovered and the number of recurrences or outbreaks a person can have may vary.
When symptoms occur soon after a person is infected, they tend to be severe. They may start as small blisters that eventually break open and produce raw, painful sores that scab and heal over within a few weeks. The blisters and sores may be accompanied by flu-like symptoms with fever and swollen lymph nodes.
Herpes most commonly can have UTI-like symptoms and people with their first outbreak experience difficult and painful urination, in addition to blisters, low grade fever, swollen lymph nodes which all point to herpes, rather than a UTI.
Sores may be a clear giveaway that you are dealing with herpes rather than a UTI, but diagnosing chlamydia and gonorrhea can be a bit trickier since STIs infecting the urogenital tract (being the organs or functions of excretion and reproduction), such as gonorrhea and chlamydia, when symptomatic, are more likely to share symptoms with UTIs.
The Herpes virus is very common and many people consider HSV-1 more benign, but it turns out there’s not much difference between the two types of virus. While it’s true that HSV-2 is a sexually transmitted disease (STD) and can cause genital sores or blisters, type 1 can do the same thing.
One big misconception is that cold sores are caused by HSV-1 and genital herpes are always type 2, but that’s not always the case.
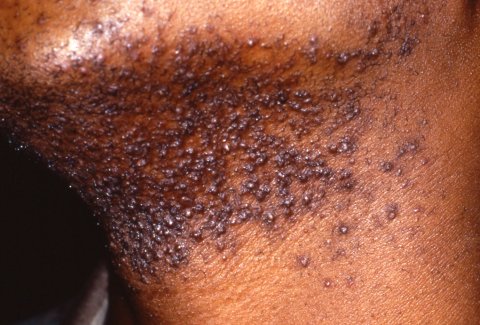
How can this be prevented?
Going for certain tests such as a urinalysis a urine culture, or a full STI screen can be administered to determine what health issue you’re actually dealing with that one can receive appropriate medical treatment.
An example, when gonorrhea has infected the urethra and does cause symptoms, they are usually painful, frequent and urgent urination and distinguishing UTI symptoms from a possible STI in your urinary tract will require a consult with your physician.
Cold sores are so common they ha ve been normalized at this point. But genital herpes is sometimes the exact same virus just in a different location.
Not only is herpes incredibly common but it’s also totally manageable. Allow us to set your mind at ease and debunk three widespread herpes myths.
It turns out you can have herpes without knowing it, even in a monogamous relationship. That’s because even if there are no noticeable symptoms like small red bumps, white blisters, pain, or itching, you can still spread the viral cells and unknowingly infect a partner.
The herpes virus is the most infectious just before, during, and after an outbreak — when blisters are present. But it also has ‘silent shedding’ between outbreaks, meaning the virus can spread at just about any time. And intercourse isn’t the only way to contract this sexually transmitted infection, often called an STI by clinicians. “The majority of new infections are HSV-1, passed from one person’s mouth to another person’s genitals during oral sex.
A lot of people are completely dumbfounded when they’re diagnosed because they did not know they could get HSV-1 on their genitals from oral sex.
Condoms can reduce the risk of herpes if they’re used correctly during vaginal, anal and/ or oral sex, but they’re not foolproof. Herpes can be spread via skin to skin contact in areas that are not covered.
Treatment for herpes/ homes remedies
The symptoms are similar and you can have more than one thing going on at a time but one tell-tale sign you have an STI, rather a UTI, is vaginal discharge.
STIs like Trichomoniasis, gonorrhea and chlamydia can present with a vaginal discharge and this will not be a symptom of a UTI in that a vaginal discharge can be completely healthy depending on the odor and color of the discharge, as well as the presence of other symptoms and it could be a sign you have an STI or vaginosis.
It also is important to distinguish between pelvic pain released when urinating with a UTI versus when the urine hits the vaginal skin wall. Obviously, if one is experiencing pain and burning, it may be hard to decipher the cause of the pain unless a trip to the doctor will give a definitive answer.
An untreated STI can lead to chronic pain, pelvic inflammatory disease with the exception of herpes, and infertility. Even if you feel in tune with your body and physical health, seeing your obstetrician or gynecologists is almost always necessary to get the proper diagnosis.
Whether it’s an STI or UTI or both, seeking medical treatment as soon as you start experiencing symptoms is paramount. Many people think you can treat a UTI by hydrating or drinking cranberry juice, but it’s an infection that requires antibiotics and if left untreated, UTIs can progress to a serious kidney infection.

